Trying to figure out what your agency’s Medicare reimbursement might look like in 2023 under the proposed rule for home health?
SimiTree’s data analysts are crunching numbers from the Centers for Medicare and Medicaid Services (CMS) to gain a better understanding of how the payment rule will impact agencies. Payment calculation changes set out in the proposed rule have been applied to 2021 data to create a model for anticipated 2023 reimbursement.
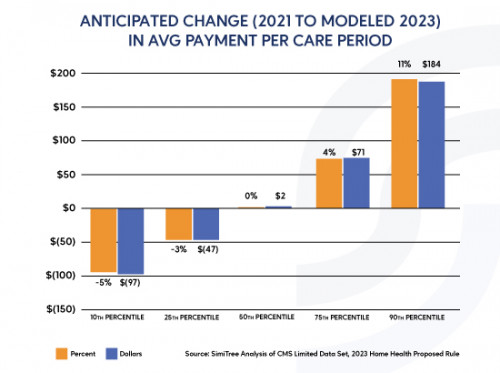
Early work with the data indicates many agencies should expect to see relatively small differences between what they were paid in 2021 and what they will be paid in 2023.
“The projection is that half of all agencies will see somewhere between a 3% decrease and a 4% increase in Medicare reimbursement,” said Christine Lang, Director of Data Analytics.
“However, it’s worth noting that the actual 2021 reimbursement reflects payment penalties, such as those for late submission of no-pay RAPs, and almost all agencies should expect a lower average case weight for non-LUPA care periods in 2023 compared to 2021,” she said.
“Further, the projections from CMS don’t take into consideration any changes in admission volume or patient characteristics or care needs and those factors can have a significant impact on agencies’ results.”
Nationally, CMS is projecting roughly a 1% decrease in total spend.
Despite those modest projections, Lang said it is important to note that most agencies will see notably smaller payments compared to reimbursement they are receiving in 2022, largely due to a decrease of more than 6% in the base payment rate.
Medicare’s base payment rate will drop from $2,031.64 in 2022 to $1,904.76 in 2023 if the payment rule is finalized as proposed.
SimiTree data analysts are readying the numbers to assist agencies with individual analyses of the expected financial impact of the proposed rule, using the data acquired from CMS.
“CMS is applying multiple changes to the underlying calculations that ultimately determine payment for home health services,” Lang said. “They are tweaking how diagnoses map to clinical groups, LUPA thresholds for some HHRGs, the wage index for many CBSAs, how OASIS answers earn points toward the functional impairment score, and how points translate to levels. Plus, they are lowering the base payment. All of the changes happening at the same time make it very difficult for an agency to anticipate and plan for reimbursement in 2023.”
Interested in an analysis?
If you are interested in a custom view of the expected impact of the proposed rules on your agency specifically, SimiTree would be happy to work with you to create a focused analysis and offer targeted recommendations.
Use the form below to reach out to us.