What is GUIDE and What Providers Need to Know
Announced on July 31, 2023, this voluntary nationwide initiative aims to provide comprehensive support for individuals living with dementia and their unpaid caregivers. Let’s delve into the key aspects of the GUIDE Model and how it's set to make a positive impact on patients and providers. For more in-depth information, be sure to visit CMS's official website. Read our blog to catch up on GUIDE now: Guiding an Improved Dementia Experience (GUIDE) Model: Revolutionizing Dementia Care » SimiTree (simitreehc.com)
In this blog post, we break down how to apply, FAQs, benefits of applying, how to get paid, and more. Keep reading for useful links and remember that our team of experts is here to help you through every step of the process. As of November 30, 2023, providers have 60 days left to apply.
GUIDE Model Overview
At its core, the GUIDE Model is designed to enhance dementia care management. Its primary objectives include improving the quality of life for individuals living with dementia, alleviating the strain on their unpaid caregivers, and enabling them to remain in their homes and communities for as long as possible. To achieve these goals, the model offers a holistic approach, including care coordination, caregiver education and support, and respite services.
The GUIDE Model aligns with the Biden Administration's focus on increasing access to high-quality care and supporting caregivers, as outlined in Executive Order 14095. It also dovetails with the National Plan to Address Alzheimer's Disease, underscoring its commitment to optimizing dementia care and advancing research.
What’s New
Participants interested in joining the established GUIDE program by CMS must submit their applications promptly. The new program cycle commences in July 2024, offering an opportunity to participate in this innovative dementia care initiative.
Who Can Participate in GUIDE?
Are home health and/or hospice agencies able to participate in GUIDE as standalone participants?
To participate in the GUIDE Model, a Medicare-enrolled home health agency and/or hospice must have or establish a Part B Medicare enrolled TIN that is eligible to bill under the Medicare Physician fee schedule. An organization may still apply if it has not yet completed the process of establishing a Part B Medicare enrolled TIN but must have an enrolled TIN prior to execution of the GUIDE participation agreement, which will occur in Spring 2024. Put simply, participants are anybody who has Part B enrolled providers, including primarily outpatient therapy providers, behavioral health organizations, physician practices, and palliative care providers.
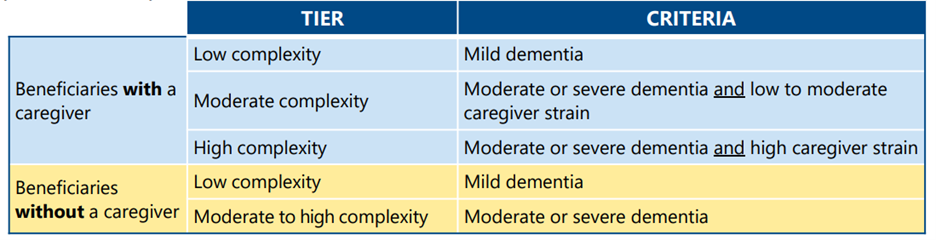
Beneficiary Tiers
Medicare beneficiaries who receive care from GUIDE participant providers will be placed in one of five tiers based on a combination of their disease stage and caregiver status. Beneficiary needs, and correspondingly, care intensity and payment, increase by tier.
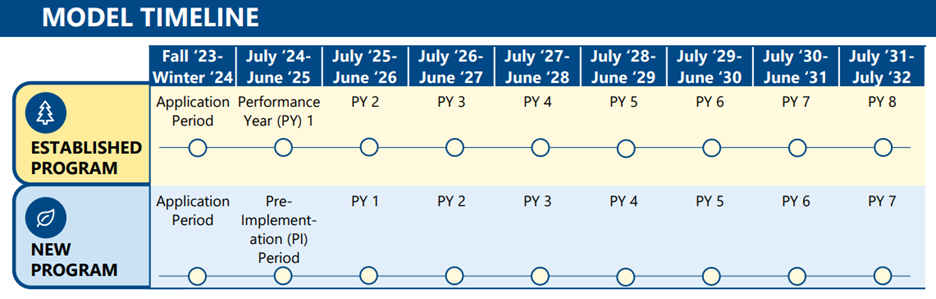
Below, you can review the GUIDE Model timeline, which you will need to reference for application and implementation period information as well.
How to Apply
GUIDE Program Application Periods
-
- Fall 2023 to Winter 2024: Providers interested in joining the GUIDE program for the new program cycle, which begins in July 2024, can submit their applications during this period.
- July 2024 to June 2025: This marks the pre-implementation period for new programs and the first performance year for established programs. During this time, new programs will prepare for their official launch in July 2024, while established programs will focus on meeting program requirements and delivering high-quality dementia care.
GUIDE Program Duration
The GUIDE program runs for eight years, providing ample time for participating providers to make a significant impact on the lives of individuals with dementia and their families.
Application Process
To participate in the GUIDE program, providers must complete an extensive application process that assesses their readiness to deliver the program's comprehensive dementia care services. The application includes a thorough review of the provider's organizational structure, staffing, experience, and financial capacity.
Benefits of Participating
The GUIDE program offers numerous benefits to participating providers, including:
-
- Access to valuable training and resources to enhance dementia care expertise
- Opportunities to collaborate with other providers and share best practices
-
- Financial support to implement and sustain the GUIDE program
- The chance to make a positive difference in the lives of individuals with dementia and their families
How to Apply for the GUIDE Program
Providers interested in joining the GUIDE program can find detailed application information and eligibility criteria on the CMS website.
The deadline for application submissions for established programs will be January 30, 2024. Read full FAQs here. RFA link: https://www.cms.gov/files/document/guide-rfa.pdf
How Do I Enroll in Medicare Part B to Become a Provider?
You can find more information about becoming a Medicare Part B provider on CMS’s website at https://www.cms.gov/medicare/enrollment-renewal/providers-suppliers/chain-ownership-system-pecos
Becoming a provider can take anywhere from a month to three months. For more information, click here to see the full fact sheet.
Also, Need to Know:
There is a requirement for 24/7 availability through a helpline. GUIDE participants shall provide either 24/7 access to an interdisciplinary care team member or maintain a 24/7 helpline that the beneficiary and/or their caregiver may call to speak with either a member of the care team or a third party engaged by the GUIDE participant to provide communication with human support (e.g., not artificial intelligence) during off-duty hours.
A third party engaged by the GUIDE Participant to provide communication during off-duty hours shall share with the interdisciplinary care team information of any communication with a beneficiary and/or their caregiver.
How Do I Get Paid with GUIDE?
The GUIDE Model will pay participants in three ways:
- Infrastructure payment: New programs may be eligible to receive an infrastructure payment of $75,000. This payment is intended to cover some of the upfront costs of establishing a new dementia care program.
- Monthly rates by tier: Participants will receive a monthly payment for each beneficiary they serve. The amount of the payment will depend on the tier of care the beneficiary is receiving. There are three tiers:
- Tier 1: Low-Intensity Care
- Tier 2: Moderate Intensity Care
- Tier 3: High Intensity Care
- Respite services: Participants will be paid for respite services provided to beneficiaries. Respite services are short-term care that allows caregivers to take a break from caring for their loved ones. The GUIDE Model will pay for respite services provided in three settings:
- In-home respite services
- Adult daycare services
- 24-hour facility services
Participants will use a set of new G-codes created for the GUIDE Model to submit claims for the monthly DCMP and the respite codes. Each model tier will have a different DCMP rate to reflect the fact that covered services and care intensity will vary across the tiers. Respite services will be paid up to an annual cap of $2,500 per beneficiary and will vary in unit costs depending on the type of respite service used.
What is the Infrastructure Payment?
Participants in the new program track who are classified as safety-net providers may be eligible to receive a one-time infrastructure payment of $75,000 to cover some of the upfront costs of establishing a new dementia care program paid at the beginning of the pre-implementation period. The infrastructure payment is intended for providers who want to develop new dementia care programs to serve underserved beneficiaries but need resources to get started. Read more about "safety net provider" and infrastructure payments here: GUIDE Model Frequently Asked Questions | CMS.
What Do the GUIDE Respite Services Include?
Per CMS, the GUIDE Model provides payment for respite services provided in three types of settings up to an annual cap of $2,500 per beneficiary. The three types of settings covered by the GUIDE Model are respite services provided in the beneficiary's home, in an adult day center, which includes both medical and social programs, and in a 24-hour facility. GUIDE participants are required to make in-home respite services available, either directly or by contracting with a provider of in-home respite.
How SimiTree Can Help
The GUIDE Model is a complex initiative, and SimiTree can help agencies of all sizes navigate its requirements and optimize their participation. Our team of experts has a deep understanding of the model and can provide tailored support to meet your agency's specific needs.
- We can provide support with our subject matter experts on Part B enrollment, creating policies for this program, and identifying/working on tools to identify beneficiaries who would benefit from this.
- We can help you evaluate and assess your EMR needs and optimize your EMR/EHR.
- We can provide general support by becoming an extension of your team, from implementation to ongoing assistance and process improvement.
- We offer training, education, and development.
Schedule a Consultation Today!
If you are interested in learning more about how SimiTree Consulting Services can help your agency participate in the GUIDE Model, please do not hesitate to call us today at 866.839.5471 or fill out a quick consultation form. We would be happy to answer your questions and discuss your specific needs.
USEFUL LINKS
- GUIDE Model Press Release
- GUIDE Model Fact Sheet (PDF)
- GUIDE Model Participant Incentives to Participate Fact Sheet (PDF)
- GUIDE Model Request for Applications (RFA) (PDF)
- GUIDE Model Frequently Asked Questions
- Webinar: GUIDE Model Overview Webinar (August 10, 2023)
- Slides (PDF) | Transcript (PDF) | Recording (MP4)

